Australia/Israel Review, Featured
Virus versus Vaccines
Aug 24, 2021 | Ahron Shapiro

Lessons from Israel’s fourth COVID-19 wave
In the fight against COVID-19, Israel was the first country to mass vaccinate its population, beginning in December 2020, inoculating 80% of adult Israelis by early August 2021. By early June 2021, it became the first to nearly eliminate the spread of the virus through the use of those vaccines.
Today, it’s the first vaccinated country to wrestle with a major resurgence of cases spurred on by spread of the Delta variant of the virus, with over 8,000 new cases a day by mid-August. It’s also the first country to take the gamble to fight the Delta flood through a lightning rollout of booster shots for the middle-aged, elderly, and more vulnerable populations, even before medical studies have weighed in on the effectiveness of such a move. By Aug. 16, over a million Israelis had received a Pfizer booster shot.
While hounded at times by setbacks, Israel’s gritty and determined path through the pandemic has given the world much to observe and learn from across a variety of aspects of the COVID-19 battle. These include its early adoption of a national vaccination strategy; the efficiency and shortcomings of its vaccine rollout; the country’s readiness to share medical data about the effectiveness and side effects of vaccines; and Israel’s emerging biotech solutions for the prevention, detection and treatment of COVID-19 globally.
Israel’s successful pitch to trial Pfizer’s mRNA vaccine on a national scale is a story that is already widely known. “[Pfizer] guaranteed enough supplies to vaccinate [Israel’s] entire population in exchange for clinical data on how the jab fared in the real world,” wrote the Financial Times’ David Crow this month. “Israel has since become a lodestar, not just for Pfizer but for public health officials across the world.”
Indeed, Australia’s selection of Pfizer as perhaps our most trusted vaccine has added additional value to Israel’s data sharing on our shores.
Israel endured three lockdowns over the course of the pandemic, costing the country’s economy an estimated 200 billion shekels (A$85 billion), the last ending in February of this year. A lockdown has been avoided since Prime Minister Naftali Bennett succeeded Binyamin Netanyahu in June, despite a major outbreak of new Delta strain cases.
In opposition, Bennett had been an outspoken critic of lockdowns, and he remains unequivocal about his preference to steer Israel through the current Delta wave without having to resort to another one.
“The Delta wave is sweeping the whole world right now, and also the State of Israel,” Prime Minister Bennett said on Aug. 15. “The State of Israel is facing the peak of morbidity in the coming weeks. We can defeat the [COVID-19] plague with two main tools: masks and vaccines. Whoever gets vaccinated saves another business, whoever gets vaccinated prevents another child from sitting for a year in front of Zoom, therefore, go out and get vaccinated and wear masks.”
“The previous government tried all the restrictions – three closures and spent NIS 200 billion,” Health Minister Nitzan Horowitz told Israel’s Reshet Bet radio station on Aug. 15. “We’re sizing up the [latest] outbreak and fighting with mass vaccinations, in a large and powerful operation. We are also increasing restrictions and hope these measures will help us prevent closure.”
Those restrictions include the reinstatement of Israel’s Green Pass system which bars unvaccinated, untested or unrecovered Israelis from attending large gatherings. The country has also tightly regulated international travel again and required quarantine for incoming travellers from all but 10 countries.
The Director-General of Israel’s Ministry of Health, Prof. Nachman Ash, told Israeli media that the effects of the booster campaign will be closely monitored as the country moves closer to the start of the school year in early September and the month-long Jewish High Holiday season beginning on Sept. 5. If the infection rate does not slow sufficiently, he said, a lockdown will become unavoidable and the start of the school year may be delayed.
With respect to the school year, Israel is planning an innovative five-step plan to avoid abandoning on-site learning even if new COVID cases continue to spread: rapid antigen testing before the first day of class; serological tests for antibodies to identify students who have already had the virus and may have better immunity; special protocols for containing an infection from spreading throughout a school without necessarily closing down classes for the uninfected, behavioural modifications; and, of course, vaccinations.
Source: Haaretz
A focus on the unvaccinated and under-vaccinated
Besides providing booster shots to older and vulnerable Israelis, and imposing new restrictions and border controls, Israeli health authorities are focusing their attention on the approximately 1.1 million eligible Israelis who are still unvaccinated.
As Prof. Ran Balicer, head of a committee of experts advising the Health Ministry on the pandemic, told Ha’aretz on July 26, “What is clear is that the chances of vaccinated people getting infected is lower than those who are not vaccinated, and that if they do get infected, their chances of serious illness are lower.”
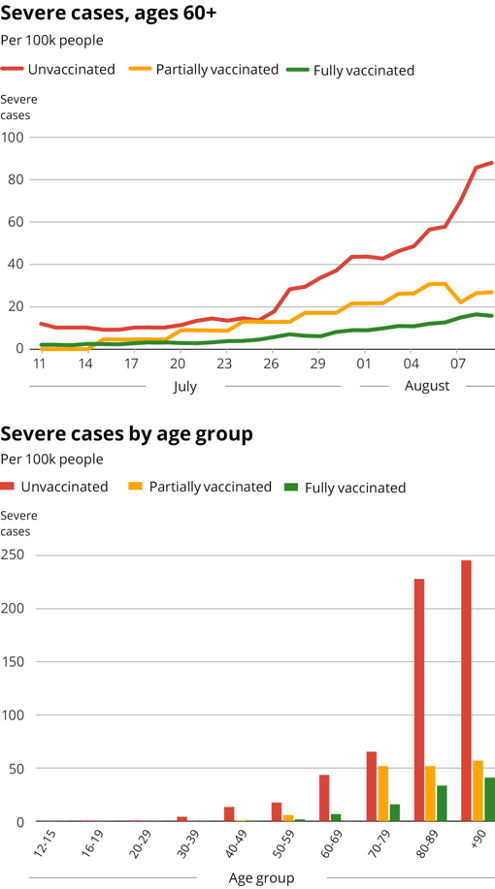
In the current wave, unvaccinated Israelis have been shown to be up to six times more likely to contract serious illness from COVID than their vaccinated counterparts. As of Aug. 10, Israeli Health Ministry data showed that among Israelis aged 60-plus, there were 16.6 people per 100,000 in serious condition. For the unvaccinated, the number was 98.5 out of 100,000.
Health Ministry officials identified three groups of Israelis that were lagging in vaccinations in comparison with the rest of the country: Israeli Arabs, ultra-Orthodox Jews, and younger Israelis in their teens and twenties.
Prof. Bishara Bisharath, chairman of the Society for the Advancement of Health in Arab Society, placed part of the blame on fatalism endemic to Arab culture, telling Israel’s Channel 12: “In the Arab sector there is a belief in fate – ‘everything is written’ [pre-determined by fate] and therefore there is hesitation to go get vaccinated,” he said.
However, Bisharath noted, Arabs were more likely to follow the advice of doctors than politicians or government officials.
“The impact of the medical staff treating them directly can have an impact. We encourage physicians to be health leaders, enlisting all of their leadership talents is the way to succeed,” he said. “We tried it in east Jerusalem. We talked to doctors and we told them it was our responsibility [to persuade patients to vaccinate]. Within a month, there was a huge change.”
Vaccination rates are particularly low among Bedouins in the Negev Desert, partly because of distrust of authorities, but also because of lack of access to vaccination hubs near their far-flung communities.
Predominantly ultra-Orthodox towns and cities also figure prominently on the list of under-vaccinated cities. According to the Health Ministry, in places like Modi’in Illit, Elad, Ganei Modi’in and Beit Shemesh only about 30% of the population had even the first dose of vaccine – although officials said the situation may not be as grave as it appears since many ultra-Orthodox have already had COVID-19 in the past and could fare a bit better than those who have never been exposed to the virus.
As mentioned before, younger Israelis are lagging in vaccinations, generally by choice, as the Times of Israel reported on Aug. 10:
“Nationally, some 90.2% of Israelis age 90-plus are vaccinated with at least two shots, and for the 80-89 age group the figure is 91.5%. It is even higher, 93.1%, for people in their 70s. But the rates decline among younger age groups: 87.2% for people in their 60s; 84.6 for people in their 50s and 81.2% for people in their 40s.
“For Israelis in their 30s and 20s, the rates are 77.8% and 72.4% respectively. The 16-19 age group is only 68% vaccinated, and only 26.2% of 12- to 15-year-olds are fully vaccinated.”
A moral dilemma
Israel’s booster shot program is not without controversy. The World Health Organisation’s position is for countries to avoid revaccinating while there are other countries (Australia among them, but especially third-world countries) that have not completed their initial vaccination drives and are short of supply.
Deputy Director of Shaare Zedek Medical Centre Prof. Dan Turner is among the prominent Israelis who have refused a booster on these grounds. And yet Turner stresses that this is simply a personal choice that every Israeli must make on their own.
And yet, here again, Israel – which saw its surplus vaccines rejected by the Palestinians in June only to have South Korea gratefully accept them – is only going through the moral dilemmas that other mostly-vaccinated countries like the United States and Canada are themselves soon approaching as the efficacy of initial vaccine doses may begin to wane. Both of those countries approved booster shots for their most vulnerable little more than a month after Israel did so.
Forward thinking
The most promising future – not only for Israel, but the world – may lie in Israeli biotech innovations that are giving the world better tools to prevent infection and fight off the deadliest complications of COVID-19 for those who contract it.
While an entire article could be devoted to this topic alone, here are just a few examples:
• Israeli-developed Enovid Nitric Oxide Nasal Spray (NONS), which has just come on the market, targets the nasal cavity, where infection usually takes place, creating an environment where the virus has no chance to infect the body.
• The Israeli company Redhill has been working on an oral antiviral treatment Opaganib, designed to supercharge the body’s defences against the virus and prevent its initial spread. Phase three trials have been completed and the company is expecting to release a report on them in the coming weeks.
• In terms of treatment for COVID-19 patients, researchers at the Hebrew University of Jerusalem have reportedly identified 18 drugs that may reduce the deadliest symptoms of COVID.
• Israeli labs have also been working on their own vaccines, like the government-funded Israel Institute for Biological research’s BriLife vaccine, which is being designed to be more resilient against COVID-19 mutations, present and future.
But arguably the most ambitious and revolutionary Israeli vaccine in development may be Oramed’s Oravax oral COVID vaccine, currently in its first clinical trial.
The capsule is not only designed to be stored at room temperature making it ideal for rollout in third-world regions, but it is also designed to target multiple parts of the virus, potentially making it more effective against new variants.
“[A] vaccine comes to you in the mail, you take it, you’re done,” Oramed CEO Nadav Kidron told AFP in an interview on Aug. 1, “Imagine.”
Tags: coronavirus, COVID-19, Israel






